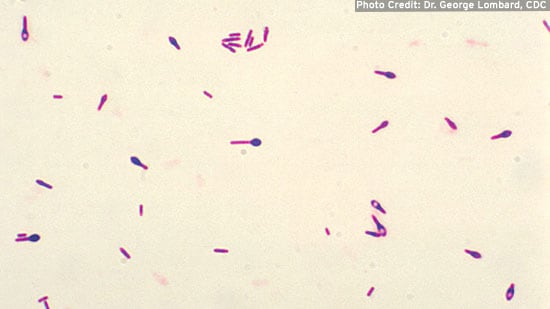
C. botulinum
What is C. botulinum?
Clostridium botulinum (C. botulinum) is a spore-forming bacterium that produces a very powerful neurotoxin that causes botulism. The toxin is among the most toxic of all naturally occurring substances. Botulism is usually associated with consumption of the toxin in food. However, in rare cases the toxin can be produced in infected wounds or in the intestinal tracts of young infants.
C. botulinum spores can be found in soil and are very resistant to heat and other treatments. Because naturally occurring levels of spores are low, growth is required to produce toxin. C. botulinum grows under anaerobic (no oxygen) conditions.
WHAT ARE THE SYMPTOMS?
Symptoms usually develop within 12 to 36 hours after consumption of contaminated food. They include double or blurred vision, slurred speech, muscle weakness and flaccid paralysis that progresses down from the head, affecting the rest of the body. Paralysis of the respiratory system may eventually cause death if not treated.
Infant botulism progresses in a different manner. The initial sign is constipation, followed by lethargy, inability to feed, floppiness and ultimately, respiratory failure. Infant botulism is rare and symptoms often take weeks to occur after consumption of spores, which grow and produce toxin in the infant’s intestine. As infants get older, they develop “healthy” bacteria in their intestine that prevent the growth of the organism. Wound botulism occurs when C. botulinum cells infect a wound and grow, producing toxin, which is carried to other parts of the body in the bloodstream.
Treatment includes removal of the toxin from the body through clearing contents of the stomach and intestine and administering antiserum. Prolonged supportive care, including artificial breathing with use of a ventilator, is required in about 80 percent of cases. Botulism has a mortality rate usually less than 10 percent, assuming treatment is promptly administered. Recovery takes weeks to months.1
HOW IS IT TRANSMITTED?
Foodborne botulism is the most common route for transmission. With a wide distribution of spores in nature, there can be low levels of contamination in agricultural products and in seafood. Outbreaks frequently involve canned foods, due to under-processing or can leakage. However, non-canned products that were subjected to temperature abuse have also been implicated, such as garlic in oil, baked potatoes, smoked fish and pasteurized carrot juice.
Honey can be contaminated with C. botulinum spores, and is the most commonly implicated food in cases of infant botulism. Honey should not be fed to infants less than 1 year of age.
HOW IS C. botulinum CONTROLLED?
Control of C. botulinum in food products requires destruction of the spores through processing or prevention of growth through formulation, temperature control, or a combination of these factors.
A commercial canning process that delivers a standard “botulinum cook” or “12D process” offers a substantial margin of safety by inactivating 12 logs of contaminating C. botulinum. For many canned products, processes that exceed a bot-cook are necessary to prevent spoilage. More recently, alternative processes are being evaluated to improve product quality. Highly trained thermal process authorities must be involved with the development of such processes to assure not only safety, but commercial sterility. Home canning processes need the same degree of stringent control.2
The goal of formulation is to prevent spore germination and outgrowth. C. botulinumdoes not grow below pH 4.6 or water activity value below 0.94, and is inhibited by certain preservatives such as sodium nitrite. A combination of these can be used to control C. botulinum growth. Low-acid products (pH >4.6) need careful handling to ensure that their thermal process inactivates C. botulinum. Although the toxin is heat labile and can be destroyed by cooking, inactivation by cooking should not be used as a control strategy for processing.
Temperature, if strictly controlled, can also be used to control C. botulinum growth. However, refrigerated products that rely solely on temperature for safety have been involved in botulism outbreaks. For example, an outbreak was associated with garlic in oil that was not properly refrigerated.3 As a result of that outbreak, the U.S. FDA requires that garlic in oil be acidified to less than pH 4.6. Botulism has only rarely been associated with dairy products, including an outbreak attributed to temperature-abused mascarpone cheese in Italy.4 Pasteurized, refrigerated carrot juice was also involved in a botulism outbreak in 2006. Temperature abuse was suspected, since the type of toxin involved cannot be formed at temperatures less than 50°F (10°C). The U.S. FDA now recommends that low-acid juices, such as carrot juice, include factors that will control C. botulinum, such as processing or pH <4.6, in="" addition="" to="">5 Smoked fish has also been involved in botulinum outbreaks. The strains sometimes associated with seafood (non-proteolytic strains) may grow at lower temperatures (39°F; 4°C) than proteolytic strains, but have higher water activity requirements (0.97).6 Spores will survive freezing and are more resistant to irradiation than many other bacteria.
For assistance with this topic or other food safety questions for your operation, Contact Us.
REFERENCES AND FURTHER INFORMATION
1CDC information
2Home canning guidance -http://www.uga.edu/nchfp/
3Solomon, H.M. and Kautter, D. A. 1988. Outbreak and toxin production by Clostridium botulinum in bottled chopped garlic. J. Food Protection 51(11):862-865.
4Aureli, P., et.al. 2000. An Outbreak in Italy of Botulism Associated with a Dessert Made with Mascarpone Cream Cheese. European Journal of Epidemiology 16(10):913-918.
5FDA CFSAN. 2007. Guidance for Industry - Refrigerated Carrot Juice and Other Refrigerated Low-Acid Juices.
6International Commission on Microbiological Specifications for Foods. Microorganisms in Foods5, Characteristics of Microbial Pathogens. Blackie Academic and Professional, New York. 1996. pages 66-111.


